Acute Brain Injury Evidenced by Decision to Cool Baby
The medical negligence attorneys at Hixson & Brown have represented numerous infants who suffered a brain injury at birth due to medical malpractice. Based on advancements in medicine, many of these severely injured infants now undergo “head cooling”, “whole body cooling” and hypothermia to treat the injury caused by lack of oxygen or birth asphyxia. If your baby has suffered a brain injury at birth or has undergone hypothermia treatment or head cooling, contact the birth injury attorneys at Hixson & Brown to seek advice as to your child’s legal rights.
Birth injuries include injuries to an infant’s brain as a result of lack of oxygen. A lack of oxygen is a condition known as asphyxia. If an event occurs during labor and delivery that causes a disruption of oxygen delivery to your unborn baby, such an event can lead to a diagnosis of Hypoxic Ischemic Encephalopathy (HIE) or Periventricular Leukomalacia (PVL). If the event causing the lack of oxygen is severe, but short lived, your child may suffer damage to his or her basal ganglia, thalami or brain stem. These areas of injury may also be referred to by the physician as “deep grey matter” injuries. However, if the event causing the lack of oxygen results in only a partial reduction in oxygen delivery, but occurs over a long period of time (ie: > 1 hour), your child may suffer damage to the periventricular or white matter of his or her brain. Both can lead to a diagnosis of Cerebral Palsy as well as significant and lifelong suffering for your child and your entire family.
According to the National Institute of Child Health and Human Development (NICHD):
Hypoxic ischemic encephalopathy (HIE) is a … life threatening condition characterized by brain injury due to asphyxia diagnosed at or shortly after birth. According to the World Health Organization, more than 722,000 children died from birth asphyxia and birth trauma worldwide in 2004. An estimated 5075 percent of infants with severe (stage 3) HIE will die, with 55 percent of these deaths occurring in the first month. Up to 80 percent of infants who survive stage 3 HIE develop significant long term disabilities, including intellectual disabilities, epilepsy, and cerebral palsy with hemiplegia, paraplegia, or quadriplegia; 10 -20 percent develop moderately serious disabilities; and up to 10 percent are normal.
Previous studies have shown treatment with hypothermia to be an effective therapy for HIE. Currently, infants diagnosed with HIE at less than six hours of age are given whole body cooling, decreasing their core body temperature to 33.5°C (93.2° Fahrenheit) for a period 72 hours using a cooling blanket. This treatment appears to protect the brain, decreasing the rate of death and disability and improving the chances of survival and neurodevelopmental outcomes at 18 months correct age.
See, Optimizing (Longer, Deeper) Cooling for Neonatal Hypoxic Ischemic Encephalopathy (HIE), https://clinicaltrials.gov/ct2/show/NCT01192776.
From a legal standpoint, the fighting issue in many of these cases is what is referred to as “causation.” Meaning, what really caused the brain injury. The physician and hospital will almost always tell the parents that the cause of the brain injury was something that happened during gestation and that “this just happens” and “we don’t’ know why.” However, the fact is that many such brain injuries happen as a result of negligent care by the physician, obstetrical nurses or the hospital during labor and delivery. Many of these injuries are preventable.
“Head cooling” or “whole body cooling” (a/k/a/ hypothermia) in the treatment of a newborn baby can be a major indicator that a child’s brain injury was the result of an acute event occurring during labor and delivery and not some remote event that occurred while the baby was growing. Medical research has shown that there are specific phases that take place after a hypoxic event (lack of oxygen) has occurred. As reported by Gunn, et al. in Hypothermic Neuroprotection, The American Society for Experimental Neurotherapeutics, Inc, Vol. 3, pp. 154-169 (4/2006):
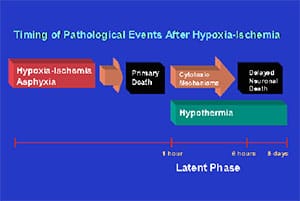
FIG. 1. Flow diagram illustrating the relationship between the phases of cerebral injury after a severe reversible hypoxic-ischemic insult. During reperfusion after the insult, there is a period of approximately 30 to 60 minutes during which cellular energy metabolism is restored, with progressive resolution of the acute cell swelling secondary to hypoxic-depolarization. This is followed by a latent phase. During this phase the intracytoplasmic components of apoptosis are activated, and the early inflammatory reaction is initiated, with induction of cytokines. This may be followed by secondary deterioration leading to ultimate delayed neuronal death after 3 days. As indicated by the bar, treatment with cerebral hypothermia needs to be initiated in the latent phase before the onset of secondary deterioration, and then continued for over 48 hours for long lasting neuroprotection.
As further stated in Neonatal Encephalopathy: Treatment and Hypothermia, by Shankaran, Journal of Neurotrauma, Vol. 26: pp. 437-443 (3/09):
The interval between primary and secondary energy failure represents a latent phase that corresponds to a therapeutic window. Initiation of therapies during the latent phase in perinatal animals has been successful in reducing brain damage and substantiates the presence of a therapeutic window (Gunn et al., 1997, 1998, 1999). The duration of the therapeutic window is approximately 6 h in near-term fetal sheep based on the neuroprotection associated with brain cooling initiated at varying intervals following brain ischemia.
Thus, when an acute hypoxic event (acute oxygen deprivation) has occurred, there is a window of up to 6 hours when head cooling or whole body cooling must be initiated.
Based on these studies of the neuroprotective effect of head cooling or whole body cooling on oxygen deprived infants, the National Institute of Child Health and Human Development (HICHD) sponsored a research trial titled: Optimizing Cooling for Neonatal Hypoxic-Ischemic Encephalopathy in 2010. Eligibility and criteria for inclusion in the research trial was as follows:
Eligibility
Ages Eligible for Study: up to 6 Hours (Child)
Sexes Eligible for Study: All
Accepts Healthy Volunteers: No
Criteria
Inclusion Criteria:
Eligibility will be determined in a stepped process:
- All infants with a gestational age ≥ 36 weeks will be screened for study entry if they are admitted to the NICU with a diagnosis of fetal acidosis, perinatal asphyxia, neonatal depression or encephalopathy.
- Infants will be eligible if:
- They have a pH ≤ 7.0 or a base deficit ≥ 16m mEq/ L on umbilical cord or any postnatal sample within 1 hour of age.
- If, during this interval, they have a pH between 7.01 and 7.15, a base deficit is between 10 and 15.9 mEq/L, or a blood gas is not available, AND they have an acute perinatal event AND either a 10 minute Apgar score ≤ 5 or assisted ventilation initiated at birth and continued for at least 10 minutes.
- Once these criteria are met, eligible infants will have a standardized neurological examination performed by a certified physician examiner. Infants will be candidates for the study when encephalopathy or seizures are present. For this study, encephalopathy is defined as the presence of 1 or more signs in 3 of the following 6 categories:
- Level of consciousness: lethargy, stupor or coma;
- Spontaneous activity: decreased, absent;
- Posture: distal flexion, decerebrate;
- Tone: hypotonia, flaccid or hypertonia, rigid;
- Primitive reflexes: a) suck, weak, absent; b) Moro, incomplete, flaccid;
- Autonomic nervous system: a) pupils: constricted, unequal, skew deviation or non reactive to light; b) heart rate: bradycardia, variable heart rate or c) respiration: periodic breathing, apnea.
Many of the criteria required before hypothermia protocols will be used are indicative of a recent hypoxic event at or near the time of birth. For example, if your child is placed on a respirator to assist in breathing and his or her APGAR scores are 5 or less at 10 minutes of life, this may indicate a lack of oxygen at or near birth. In addition, if your child has cord blood gases at birth or blood gases within the first hour of life that reflect an acidosis (pH <7 or a Base Excess of 16 or more), then this is additional evidence of an acute hypoxic event at or near the time of birth. The acute nature of these finding warrant hypothermia treatment to lessen the extent of the brain damage being caused by the lack of oxygen.
If your child has been treated with “head cooling”, “whole body cooling” and hypothermia, it is possible your child suffered an acute brain injury due to lack of oxygen during the labor and delivery process. You should immediately contact an attorney who specializes in the representation of infants and families who can review the medical record and determine if medical negligence may have caused or contributed to your child’s brain injury or its severity.